Legionella is a risk when designing water systems.
Crystal IS
05/14/2019
Over the last few years, there has been a steady increase in drinking-water associated disease and outbreaks, particularly those caused by bacterial microorganisms. According to the Centers for Disease Control (CDC), a total of 42 outbreaks were reported across 19 states between 2013 and 2014. More than half of those (57 percent) were due to Legionella, a bacteria that has been determined by the World Health Organization (WHO) to be the most detrimental waterborne pathogen to human health in the developed world. While aging infrastructure and poor maintenance practices play a role in these statistics, pipes are not the only reason waterborne pathogens are on the rise.
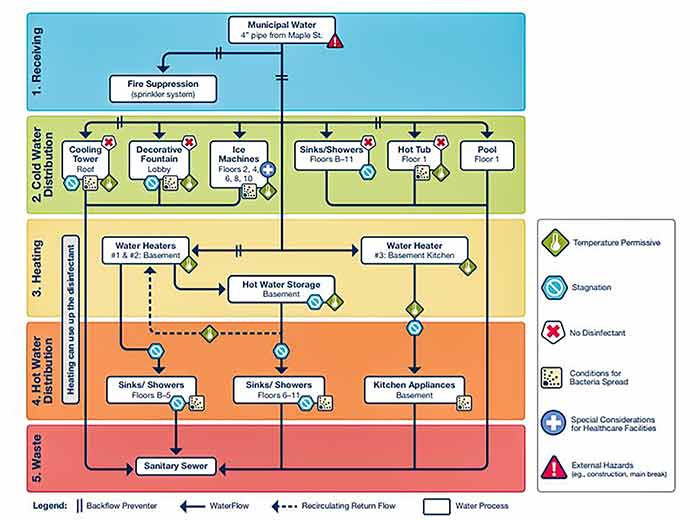 Image 1. Example of a water system design (Image courtesy of Crystal IS)
Image 1. Example of a water system design (Image courtesy of Crystal IS)
